Pharmaceutical Corruption Media Articles
Below are key excerpts of revealing news articles on pharmaceutical industry corruption from reliable news media sources. If any link fails to function, a paywall blocks full access, or the article is no longer available, try these digital tools.
For further exploration, delve into our comprehensive Health and Food Corruption Information Center.
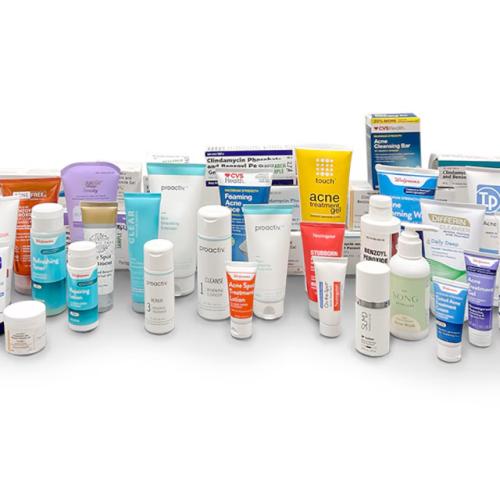
Television ads for drugs are filled with glowing images of people living their best lives, all thanks to that new med they've been prescribed. But drugs being touted on TV often have little to no benefit compared to other treatments, a new study published online Jan. 13 in JAMA Network Open finds. Fewer than one-third of drugs commonly advertised in the United States are highly rated first-line therapies, based on regulatory reviews from three different health agencies, the researchers said. Further, medications categorized as "low benefit" accounted for nearly $16 billion of the $22 billion in TV ad spending during the six-year study period, the results showed. "Proponents of direct-to-consumer pharmaceutical advertising often argue that these ads have high public health value by encouraging uptake of the most therapeutically beneficial therapies. Our study pushes back against this argument," said lead researcher Neeraj Patel. "The U.S. is one of only two high-income countries in the world that widely permits direct-to-consumer advertising of prescription drugs," Patel said. "And there's been a ton of empirical research over the past two decades that has suggested that this type of advertising can be misleading, lead to inappropriate prescribing, and inflate health care costs." In the meantime, people should have frank discussions with their doctor about any drug that's caught their eye on TV, focusing on the real risks and benefits, Patel said.
Note: This profoundly eye-opening interview of a top cardiologist reveals without doubt how big Pharma has corrupted science and greatly damaged public health. For more along these lines, see concise summaries of deeply revealing news articles on big Pharma corruption from reliable major media sources.
Vaccine-makers sought to shape content moderation actions at Twitter. Stronger, a campaign run by Public Good Projects, a public health nonprofit specializing in large-scale media monitoring programs, regularly communicated with Twitter on regulating content related to the pandemic. The firm worked closely with the San Francisco social media giant to help develop bots to censor vaccine misinformation and, at times, sent direct requests to Twitter with lists of accounts to censor and verify. Internal Twitter emails show regular correspondence between an account manager at Public Good Projects, and various Twitter officials, including Todd O’Boyle, lobbyist with the company who served as a point of contact with the Biden administration. The content moderation requests were sent throughout 2021 and early 2022. The entire campaign ... was entirely funded by the Biotechnology Innovation Organization, a vaccine industry lobbying group. BIO, which is financed by companies such as Moderna and Pfizer, provided Stronger with $1,275,000 in funding for the effort, which included tools for the public to flag content on Twitter, Instagram, and Facebook for moderation. Many of the tweets flagged by Stronger contained absolute falsehoods. But others hinged on a gray area of vaccine policy through which there is reasonable debate, such as requests to label or take down content critical of vaccine passports and government mandates to require vaccination.
Note: For more along these lines, see concise summaries of deeply revealing news articles on coronavirus vaccines and media manipulation from reliable sources.
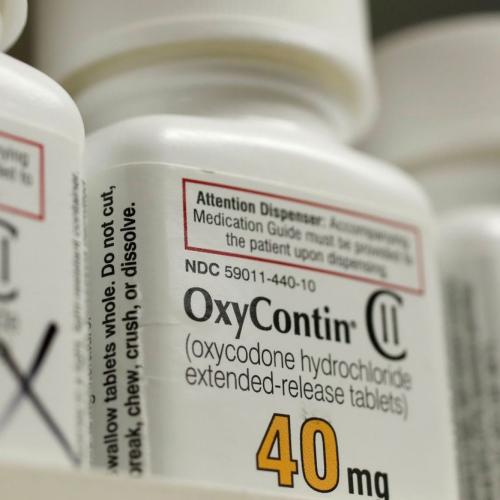
The Centers for Disease Control and Prevention (CDC) has been accused of bowing to drug industry pressure after releasing new guidelines that doctors say put lives at risk by rowing back on warnings about the dangers of opioid prescribing. The latest CDC guidelines have caused controversy after dropping specific limits on dosages and lengths of prescribing from a key summary of recommendations used by physicians. Dr Andrew Kolodny, president of Physicians for Responsible Opioid Prescribing, sees the drug industry’s hand behind the change. Kolodny has testified against opioid makers in legal actions over their part in driving the opioid epidemic by pushing sales with false claims about their safety and effectiveness. They include Purdue Pharma, manufacturer of OxyContin, a powerful narcotic pill that kickstarted the US’s opioid epidemic alongside the company’s marketing strategy to see the drugs widely prescribed. Kolody said ... that the drug industry calculated how much the 2016 CDC guidelines would cost it if doctors followed the recommendations to limit prescribing of high dosage pills. “The highest dosage products have had the highest profit margin. It only costs a few extra pennies to make the higher dosage pill, but retail it’s almost double what they get per pill or prescription. So the industry fought very hard to block the release of the 2016 guideline and when that failed they did everything they could to make the guidelines appear controversial. And that worked,” he said.
Note: For more along these lines, see concise summaries of deeply revealing news articles on corruption in government and in Big Pharma from reliable major media sources.
Scandals brought down Harvey Weinstein’s movie studio and major opioid supplier Mallinckrodt. But their wealthy owners, directors and executives were granted lifetime immunity from related lawsuits in bankruptcy court — an overwhelmingly common tactic in major U.S. Chapter 11 cases, a Reuters review found. Such immunity grants have become a pervasive but little-understood feature of the U.S. bankruptcy system. The releases are now granted by judges in 9 of 10 major Chapter 11 cases. The lawsuit shields, requested by the company or organization in bankruptcy, are called “nondebtor” releases because they are bestowed on people and entities that never have to declare Chapter 11 themselves. The recipients effectively get the benefits of bankruptcy protection without the associated financial or reputational damage. Reuters ... examined 29 U.S. bankruptcies that were preceded by mass tort litigation against companies or other entities, many of which included allegations involving dangerous products or sexual abuse. The review found that about 1.2 million claimants in these cases have signed away their rights to sue related parties or face pressure to approve such releases in ongoing bankruptcy-court negotiations. The 29 bankruptcies included those of 14 Catholic dioceses or religious orders and the Boy Scouts of America amid lawsuits alleging child molestation; [and] the collapse of opioid suppliers Purdue Pharma LP and Mallinckrodt plc over their alleged roles in a deadly addiction epidemic.
Note: For more along these lines, see concise summaries of deeply revealing news articles on corporate corruption and sexual abuse scandals from reliable major media sources.
Pfizer's plan to as much as quadruple U.S. prices for its COVID-19 vaccine next year is beyond Wall Street's expectations and will spur its revenue for years despite weaker than anticipated demand for the new booster shot so far, analysts said. The drugmaker, which developed and sells the vaccine with Germany's BioNTech, said on Thursday evening that it is targeting a range of $110 to $130 a dose for the vaccine once the United States moves to a commercial market next year. Analysts said the move could lead to price hikes by rivals. The companies have varied the pricing during the pandemic, with wealthy countries paying the most for the shots and the poorest countries the least. Wells Fargo analyst Mohit Bansal said the new pricing range for the vaccine could add around $2.5 billion to $3 billion in annual revenue for Pfizer. "This is much higher than our assumption of $50 per shot," Bansal wrote in a research note. Global vaccine access group the People’s Vaccine Alliance, which has pushed for Pfizer to allow cheaper copies of the vaccine to be made, called the proposed price hike "daylight robbery." The price range announced by Pfizer represented a more than 10,000% markup over what experts have estimated it costs the vaccine makers to produce the shots.
Note: For more along these lines, see concise summaries of deeply revealing news articles on coronavirus vaccines from reliable major media sources.
Every five years, top officials of the Food and Drug Administration go behind closed doors to negotiate the terms of its core budget – about $3 billion this year. But the F.D.A. is not at the table with members of Congress or with White House officials. Instead, it's in dozens of meetings with representatives of the giant pharmaceutical companies whose products the agency regulates. The negotiations are a piece of the "user fee" program in which drug, device and biotech companies make payments to the agency partly to seek product approvals. The fees ... make up nearly half of the F.D.A.'s budget, financing 6,500 jobs at the agency. The pharmaceutical industry funding alone has become so dominant that last year it accounted for three-quarters – or $1.1 billion – of the agency's drug division budget. Advocates for patients and doctors say the agreements have enabled the industry to weaken the approval process meant to ensure that drugs are safe and effective. "It's kind of like a devil's bargain," said Dr. Joseph Ross, a professor at the Yale School of Medicine who has studied F.D.A. policies, "that I think is not in the best interest of the agency, because it turns this every-five-year cycle into the F.D.A. essentially asking industry, 'What can we do to secure this money?'" Senator Bernie Sanders ... suggested that the pharmaceutical companies' tendency to charge "outrageous" prices was related to their significant role in funding and advancing policy goals of the F.D.A.'s drug division.
Note: A revealing interview of a top cardiologist illuminates the history of how Big Pharma has corrupted science and greatly damaged public health. For more along these lines, see concise summaries of news articles on big Pharma corruption from reliable major media sources.
The updated Covid vaccine boosters, a reformulated version targeting the BA.5 omicron subvariant [will] be the first Covid shots distributed without results from human trials. Because the Biden administration has pushed for a fall booster campaign to begin in September, the mRNA vaccine-makers Pfizer-BioNTech and Moderna have only had time to test the reformulated shots in mice, not people. That means the Food and Drug Administration is relying on the mice trial data — plus human trial results from a similar vaccine that targets the original omicron strain, called BA.1 — to evaluate the new shots. Federal health officials hope that the new vaccines will provide stronger protection over the existing booster shots, which still target the original coronavirus strain. But the lack of data in humans means officials likely won’t know how much better the new shots are — if at all — until the fall booster campaign is well underway. The FDA’s decision to move forward without data from human trials is a gamble, experts say, threatening to further lower public trust in the vaccines should the new boosters not work as intended. The U.S. is still on its first iteration of the Covid vaccines, and the mRNA technology has only been in widespread use since late 2020. The agency is making “huge assumptions” in its consideration of the new Covid boosters, [Dr. Paul] Offit said, adding that it’s possible the new shots may not be any more effective than the existing vaccines.
Note: Read a revealing article with critical information about the new mRNA boosters. To further inquire into this complex topic, explore concise summaries of news articles on coronavirus vaccines and Big Pharma corruption from reliable major media sources.
Soon after giving birth to a daughter two months premature, Terri Logan received a bill from the hospital. She recoiled from the string of numbers separated by commas. Then a few months ago Logan received some bright yellow envelopes in the mail. They were from a nonprofit group [RIP Medical Debt] telling her it had bought and then forgiven all those past medical bills. The nonprofit has boomed during the pandemic, freeing patients of medical debt, thousands of people at a time. Its novel approach involves buying bundles of delinquent hospital bills – debts incurred by low-income patients like Logan – and then simply erasing the obligation to repay them. It's a model developed by two former debt collectors, Craig Antico and Jerry Ashton, who built their careers chasing down patients who couldn't afford their bills. RIP buys the debts just like any other collection company would – except instead of trying to profit, they send out notices to consumers saying that their debt has been cleared. A surge in recent donations – from college students to philanthropist MacKenzie Scott, who gave $50 million in late 2020 – is fueling RIP's expansion. To date, RIP has purchased $6.7 billion in unpaid debt and relieved 3.6 million people of debt. RIP is one of the only ways patients can get immediate relief from such debt, says Jim Branscome, a major donor. "As a bill collector collecting millions of dollars in medical-associated bills in my career, now all of a sudden I'm reformed: I'm a predatory giver," Ashton said.
Note: To understand the corruption in healthcare that results in expensive medical bills, read this revealing 10-page summary of medical doctor Marcia Angell's book The Truth About Drug Companies. To further explore stories that help create the world we want to live in, check out our inspiring news articles collection and our Inspiration Center.
Big Pharma spent more than any other industry to lobby Congress and federal agencies this year, a Reuters analysis shows, but is still on course for a major defeat by failing to stop a bill that allows the government to negotiate prices on select drugs. The $430 billion Inflation Reduction Act to change climate, health, and tax policies cleared its largest hurdle last week when Democratic lawmakers passed it in the Senate. The U.S. House of Representatives is also expected to pass it on Friday, allowing President Joe Biden to sign it into law. A Kaiser Family Foundation poll in October found that 83% of Americans, including 95% of Democrats and 71% of Republicans, want the federal Medicare health plan for seniors to negotiate prices. The industry's powerful trade association, Pharmaceutical Research and Manufacturers of America (PhRMA), urged senators in a public letter to reject the bill. A Reuters analysis ... shows that the pharmaceutical industry has spent at least $142.6 million on lobbying Congress and federal agencies in the first half of 2022, more than any industry, and at least $16.1 million on campaign contributions during the current mid-term election cycle. Almost two thirds of the money spent on lobbying ... came from PhRMA and its member companies. The bill's provision for drug price negotiations was scaled back in November, allowing Medicare to focus on an annual maximum of 20 of the costliest medicines by 2029, instead of an initial proposal to help reduce prices for 250 treatments.
Note: For more along these lines, see concise summaries of deeply revealing news articles on corruption in government and in the pharmaceutical industry from reliable major media sources.
It's estimated that more than 107,000 people in the United States died due to opioid overdoses in 2021. Washington Post journalist Scott Higham notes it's "the equivalent of a 737 Boeing crashing and burning and killing everybody on board every single day." In the new book, American Cartel, Higham and co-author Sari Horwitz make the case that the pharmaceutical industry operated like a drug cartel, with manufacturers at the top; wholesalers in the middle; and pharmacies at the level of "street dealers." The companies collaborated with each other — and with lawyers and lobbyists — to create legislation that protected their industry, even as they competed for market share. "It really is the companies that run the show," Higham says. "People were dying by the thousands while these companies were lobbying members of Congress ... to pass legislation and to lobby members of the Department of Justice and try to slow down the DEA enforcement efforts." Big pharma fought to create legislation that would limit the DEA's ability to go after drug wholesalers. The efforts were effective; more than 100 billion pills were manufactured, distributed and dispensed between 2006 and 2014. Meanwhile, both federal and state DEA agents are frustrated by the ways in which their enforcement efforts have been curtailed. Right now there are 40,000 Americans who are in jail on marijuana charges. And not one executive of a Fortune 500 company involved in the opioid trade has been charged with a crime.
Note: For more along these lines, see concise summaries of deeply revealing news articles on corruption in government and in the pharmaceutical industry from reliable major media sources.
A group of whistleblowers has provided evidence that the Environmental Protection Agency has not adequately assessed the health risks posed by several new chemicals on the grounds that they are corrosive. Those harms include cancer, miscarriage, and neurotoxicity, according to the whistleblowers, who work as health assessors in the division. In some cases … the risks were calculated, found to be significant, and later deleted from official documents. In March 2020, Gallagher, the human health assessor, found that another chemical presented risks to workers. Information [about the hazards] was included in a version of the assessment. But a month later, a manager in the New Chemicals Division created a new assessment [that] explained: "Risks were not evaluated for workers via repeated dermal exposures because dermal exposures are not considered likely due to the corrosivity of the new chemical substance." According to the whistleblowers, this statement is false. "It is intentionally misleading for EPA to put into a report that we did not calculate risk when we did," said Martin Phillips, a chemist and human health assessor who works in the EPA's Office of Pollution Prevention and Toxics. "It's lying about what we did. It's not just that we did the calculations. We did the calculations and found risks, and then they got rid of them and said that we didn't calculate them. It's fundamentally inaccurate."
Note: For more along these lines, see concise summaries of news articles on pharmaceutical corruption and science corruption from reliable major media sources.
We urgently need a national debate about guns. But we also urgently need a national debate about the epidemic of mood-altering drugs being prescribed to young Americans. Mass shooters in the United States tend to be young, obsessive, male loners and many have been prescribed psychoactive drugs. For example, Eric Harris, one of the two shooters at Columbine High School in Columbine, Colorado, in 1999—which ushered in the current spate of mass shootings—was on the psychotropic drug Luvox. Prescribing information for the antidepressant says, “Close supervision of patients and in particular those at high risk should accompany drug therapy.” Jeff Weise, who fatally shot his grandfather, his grandfather’s girlfriend, and then seven others at the Red Lake Senior High School in Minnesota in 2005, was on the well-known antidepressant Prozac. Two years later, Cho Seung-Hui, who perpetrated the Virginia Tech mass shooting, also was found to be on psychoactive antidepressants. Jeanne Stolzer, associate professor of child and adolescent development at the University of Nebraska-Kearney, observes that “despite the multitude of international drug regulatory warnings on all classifications of psychiatric medications citing adverse reactions such as suicidal ideation, homicidal ideation, violence, and psychosis, not one local, state, or federal commission has investigated the correlation between the mass shootings in America and the use of psychiatric medications.”
Note: Although Epoch Times is often deemed as a controversial media platform, this article raises legitimate questions on an important topic seldom discussed. Read a revealing article that investigates the alarming adverse events associated with common mood-altering medications prescribed for those struggling with mental illness. For more on this concerning trend, consider exploring an in-depth article written by an anonymous doctor who reveals the decades of evidence showing how adverse reactions from psychiatric drugs can manifest as both suicides and homicides.
Today it’s my great pleasure to introduce two Pulitzer Prize-winning Washington Post journalists, Sari Horwitz and Scott Higham, who are going to discuss their new book, "American Cartel." We're talking about companies that create and fuel the opioid crisis. We've heard this story about the Sacklers and indeed the Sacklers have been identified, and if criminal charges haven't been brought at least they've been vilified in the press. But ... this goes way beyond the Sacklers. This is not just the story of one bad apple. "It's so much bigger than that," [said Horwitz]. "We found, in our two-year investigation ... a constellation of companies that fuel the deadliest epidemic, drug epidemic, in American history. Some of these companies are some of the largest in this country. Some we've heard of. They are household names - Walgreens, Walmart, Johnson & Johnson. We found internal emails from these companies where the people in the companies were laughing at the addicts. They were mocking them. Meanwhile, the drug companies, they are smart. They decide to lure away the best and the brightest if they can from the DEA and the Justice Department to help them as they are selling opioids, and they are very successful. They hired dozens of people from DEA and the Justice Department to work for these companies. So again, these are the people who are trying to protect us, working for the DEA and the Justice Department. They are lured away to the companies who are selling addictive painkillers that are killing people."
Note: For more along these lines, see concise summaries of deeply revealing news articles on government corruption and Big Pharma profiteering from reliable major media sources.
California will begin making its own low-cost insulin in an effort to make the essential diabetes treatment more affordable, Gov. Gavin Newsom announced on Thursday. “Nothing epitomizes market failures more than the cost of insulin,” the governor said in a video posted on Twitter, “Many Americans experience out-of-pocket costs anywhere from three hundred to five hundred dollars per month for this life-saving drug.” With a budget of $100 million, California plans to “contract and make our own insulin at a cheaper price, close to at cost, and to make it available to all,” Newsom said. It’s unclear exactly how inexpensive California’s insulin will be or when the low-cost drugs will be available. Insulin in the U.S. costs almost $100 per unit, on average. That’s nearly four times the price in Chile, which has the second-highest prices among the 34 countries analyzed by the nonprofit Rand Corporation, at less than $25 per unit. Currently, four in five Americans in need of insulin have incurred thousands of dollars in credit card debt to pay for the medication, according to a recent survey commissioned by health care organization CharityRx. The average debt among all survey participants was $9,000. California’s program will allot $50 million toward the development of cheaper insulin products and $50 million on an in-state insulin manufacturing facility, Newsom said, adding that the facility “will provide new, high-paying jobs and a stronger supply chain for the drugs.”
Note: The unethical corruption of big Pharma is so clearly seen in the ridiculously inflated prices of drugs in the US compared to other countries. For more along these lines, see concise summaries of deeply revealing news articles on Big Pharma profiteering from reliable major media sources.
Over the past decades, regulatory agencies have seen large proportions of their budgets funded by the industry they are sworn to regulate. In 1992, the US Congress passed the Prescription Drug User Fee Act (PDUFA), allowing industry to fund the US Food and Drug Administration (FDA) directly through “user fees.” The FDA moved from a fully taxpayer funded entity to one supplemented by industry money. Net PDUFA fees collected have increased 30 fold—from around $29m in 1993 to $884m in 2016. In Europe, industry fees funded 20% of ... the European Medicines Agency (EMA), in 1995. By 2010 that had risen to 75%; today it is 89%. Australia had the highest proportion of budget from industry fees (96%) and in 2020-2021 approved more than nine of every 10 drug company applications. But for decades academics have raised questions about the influence funding has on regulatory decisions, especially in the wake of a string of drug and device scandals—including opioids, Alzheimer’s drugs, influenza antivirals, pelvic mesh, joint prostheses, breast and contraceptive implants, cardiac stents, and pacemakers. An analysis of three decades of PDUFA in the US has shown how a reliance on industry fees is contributing to a decline in evidentiary standards, ultimately harming patients. A BMJ investigation last year found several expert advisers for covid-19 vaccine advisory committees in the UK and US had financial ties with vaccine manufacturers—ties the regulators judged as acceptable.
Note: For more on this massive legal corruption, see this article. For more along these lines, see concise summaries of deeply revealing news articles on corruption in government and in Big Pharma from reliable major media sources.
Medicare’s drug program could have saved up to $3.6 billion in 2020 by mirroring the pricing strategy of entrepreneur and Shark Tank judge Mark Cuban’s online pharmacy, according to a new study. Cuban’s Cost Plus Drug Co. offers a selection of generic drugs at the cost of manufacturing them plus a flat 15% markup. The direct-to-consumer pharmacy does not accept insurance. The study’s authors suggest that Medicare is overpaying for many generic drugs and could save billions a year if it purchased them directly from Cuban’s online pharmacy. “The lower prices from a direct-to-consumer model highlight inefficiencies in the existing generic pharmaceutical distribution and reimbursement system, which includes wholesalers, pharmacy benefit managers, pharmacies, and insurers,” wrote researchers at Brigham and Women’s Hospital and Harvard Medical School in a brief published ... in the journal Annals of Internal Medicine. Cuban and his pharmacy did not fund or have any involvement in the study. Cost Plus Drug Co. says it engages in price negotiations with drugmakers. Medicare’s drug program, Part D, however, prohibits the government from directly negotiating pharmaceutical prices. Researchers compared 2020 Medicare spending for a total of 89 drugs ... to their prices at Cost Plus Drug Co. in February. They estimate that Medicare overpaid for 77 generic drugs, spending $8.1 billion compared with $4.5 billion if the federal agency had purchased at the same prices as Cost Plus Drug Co. charges.
Note: For more along these lines, see concise summaries of deeply revealing news articles on government corruption and Big Pharma profiteering from reliable major media sources.
Public health initiatives in the United States are suffering from a crisis of trust. Recent polls show that only a third of the public trusts insurance and pharmaceutical companies, while just 56 percent trust the government health agencies that are meant to regulate these industries. Another survey during the COVID-19 pandemic showed that only around half of Americans have a "great deal" of trust in the CDC, while a mere third have such trust in the Department of Health and Human Services. When the mRNA vaccines for COVID-19 were made available to the public free of charge, a national conversation began about "vaccine hesitancy"–the phenomenon of Americans choosing not to be vaccinated even when incentivized and, in some cases, coerced. Americans had watched public health experts lie, misdirect, ignore evidence and yield to professional pressure. Few wanted to be their guinea pigs. Not all the COVID-19 gaslighting was the fault of the media or politicians - much was implemented by experts abusing their apolitical position of trust. The experts ... including Drs. Deborah Birx and Anthony Fauci, insisted on the most asinine and evidence-free preventative measures, including facial coverings, lockdowns and social distancing. Their insulated role as health advisers enabled them to manipulate health policy in ways that benefited only themselves. The most stark example was the corruption of data collection at the Center for Disease Control–a scandal that crashed public trust to a new low.
Note: For more along these lines, see concise summaries of deeply revealing news articles on government corruption and the coronavirus from reliable major media sources.
Celebrity investor Mark Cuban is receiving praise on social media after he launched a new company that provides patients access to affordable medications. Cuban launched the Mark Cuban Cost Plus Drug Company (MCCPDC), a direct-to-consumer online company that offers more than 100 generic medications at discounted prices. The investor said he aims to "be the low-cost provider of medications to patients." He continued: "If you don't have insurance or have a high deductible plan, you know that even the most basic medications can cost a fortune. Many people are spending crazy amounts of money each month just to stay healthy. No American should have to suffer or worse—because they can't afford basic prescription medications." The company's low costs are achieved by working directly with partners, which "allows us to only markup our costs by 15 percent," Cuban explained. Explaining the business model, Cuban cited the drug prescribed for hookworm, Albendazole, which can cost as much as $500 per course. "Our cost for Albendazole is $26.08 per course. We mark that price up by 15 percent so we can continue to run the company and invest in disrupting the pricing of as many drugs as we possibly can," he explained. "That makes the base price of the drug $30. Then we add on the actual cost, $3.00, that our pharmacy partners charge us to prepare and provide your prescription to you. "That makes the sales price on this website $33. Far, far lower than the pricing available in the marketplace."
Note: As big Pharma rakes in the huge profits, Marc Cuban has created a new company called CostPlus which brings many expensive drugs to you at a fraction of the price. Sadly, very few of the major media are reporting on this. Cuban says, “Everyone should have safe, affordable medicines with transparent prices.”
The prices of new drugs in the U.S. have climbed for more than a decade, a study published Tuesday finds. According to a research letter in the Journal of the American Medical Association, the launch prices of new brand-name drugs increased by nearly 11 percent every year from 2008 through 2021. “These prices are increasing far out of proportion to other health care services,” said the lead author, Dr. Benjamin Rome. Rome, and his colleagues observed price increases for all types of drugs, including cancer drugs, non-cancer drugs, pills and injections, he said. “Ultimately,” he said, “all health care costs are borne by consumers — either direct out-of-pocket costs, higher premiums or taxes in the case of public health insurance.” He added, “Insurance companies can also require prior authorization for expensive new drugs or not cover the drugs at all.” The researchers calculated the negotiable sticker prices for new drugs on the market, or the net price. Such prices, which were adjusted for inflation, were calculated in light of rebates many drugmakers offer for the drugs. The researchers limited their scope to drugs sold by public companies; the net price averages included nearly 400 new drugs in total. Median drug prices for a year’s supply increased from $2,115 in 2008 to more than $180,000 in 2021. The greatest increases were for cancer drugs and therapies used to treat rare diseases. In 2008, 9 percent of drugs cost $150,000 or more a year, compared to 47 percent in 2021.
Note: For a more detailed and eye-opening analysis, see this article. For more along these lines, see concise summaries of deeply revealing news articles on Big Pharma profiteering from reliable major media sources.
American hospitals have been living with serious drug shortages for more than a decade. Most days, nearly 300 essential drugs can be in short supply. It's not a matter of supply and demand. The drugs are needed and the ingredients are easy to make. Pharmaceutical companies have stopped producing many life-saving generic drugs because they make too little profit. Yet, year after year, the government stays on the sidelines as companies take drug production offline - and doctors worry the shortages are compromising patient care. Neonatologist Dr. Mitch Goldstein treats the most vulnerable patients. Many ... premature and sick babies have undeveloped digestive systems, so Dr. Goldstein keeps them alive with intravenous nutrients, many of which are in short supply. Antony Gobin heads the pharmacy at Loma Linda Hospital. He told us shortages of basic drugs are a constant worry. "We were dealing with shortages long before COVID," [he said]. "They're all very old, fundamental drugs that every hospital in the country needs and uses." Drug shortages can kill. In 2011, when norepinephrine, an old, low profit drug used to treat septic shock, was in short supply, hundreds of people around the country died. Middlemen, the group purchasing organizations and drug distributors take their cut. The drug manufacturers end up with just a small fraction of what the patient pays. Many have simply stopped making the least profitable drugs.
Note: For more, see this article. For more along these lines, see concise summaries of deeply revealing news articles on Big Pharma corruption and health from reliable major media sources.
Important Note: Explore our full index to key excerpts of revealing major media news articles on several dozen engaging topics. And don't miss amazing excerpts from 20 of the most revealing news articles ever published.